DE FAAKTO OUTBREAK INTELLIGENCE
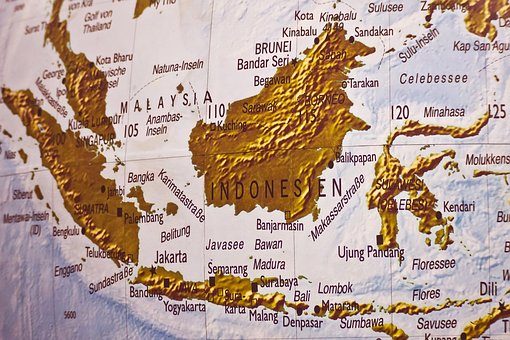
PAPUA PROVINCE INDONESIA
SITUATION-CIRCULATING VACCINE-DERIVED POLIOVIRUS TYPE 1
World Health Organization is reporting,
- On 12 February, a circulating vaccine-derived poliovirus type 1 (cVDPV1) has been confirmed in Papua province, Indonesia
- Two genetically-linked VDPV1 viruses were isolated from a child with acute flaccid paralysis (AFP) with onset of paralysis on 27 November 2018
- Even though this province shares a border with Papua New Guinea, this outbreak is not linked to the cVDPV1 outbreak currently affecting its neighbouring country
- Outbreak response immunization (ORI) has been conducted in Yahukimo district and 5718 children under 15 years of age have been immunized with bivalent oral polio vaccine (bOPV) (WHO)
WHO Risk Assessment
- The detection of cVDPVs underscores the importance of maintaining high routine vaccination coverage everywhere to minimize the risk and consequences of any poliovirus circulation as well as the need to ensure quality surveillance for early detection of any polioviruses
- The overall risk is assessed as moderate at the national level due to the sub-optimal polio vaccination coverage and surveillance quality in Papua province of Indonesia
- At the regional level despite proximity with Papua New Guinea the overall risk is assessed to be low as there is limited cross border population movement from the affected area; however, virological analysis indicates that the virus may have been possibly circulating for a few years with immunization coverage being low in neighbouring areas
- The risk of further spread of cVDPV1 within the country remains a great concern due to poor routine immunization coverage
- WHO’s International Travel and Health recommends that all travellers to polio-affected areas be fully vaccinated against polio
About Polio
- There is no cure for polio, it can only be prevented. Polio vaccine, given multiple times, can protect a child for life
- Polio is a highly infectious disease caused by a virus. It invades the nervous system, and can cause total paralysis in a matter of hours. The virus is transmitted by person-to-person spread mainly through the faecal-oral route or, less frequently, by a common vehicle (for example, contaminated water or food) and multiplies in the intestine. Initial symptoms are fever, fatigue, headache, vomiting, stiffness of the neck and pain in the limbs. 1 in 200 infections leads to irreversible paralysis (usually in the legs). Among those paralysed, 5% to 10% die when their breathing muscles become immobilized. (WHO)
- WHAT IS VACCINE-DERIVED POLIO?
A: Oral polio vaccine (OPV) contains an attenuated (weakened) vaccine-virus, activating an immune response in the body. When a child is immunized with OPV, the weakened vaccine-virus replicates in the intestine for a limited period, thereby developing immunity by building up antibodies. During this time, the vaccine-virus is also excreted. In areas of inadequate sanitation, this excreted vaccine-virus can spread in the immediate community (and this can offer protection to other children through ‘passive’ immunization), before eventually dying out - On rare occasions, if a population is seriously under-immunized, an excreted vaccine-virus can continue to circulate
- WHO’s International Travel and Health recommends that all travelers to polio-affected areas be fully vaccinated against polio
Vaccines
- There are six different vaccines to stop polio transmission:
- Inactivated polio vaccine (IPV) – protects against poliovirus types 1, 2, and 3
- Trivalent oral polio vaccine (tOPV) – protects against poliovirus types 1, 2, and 3 – following the “OPV Switch” in
- April 2016, tOPV is no longer in use
- Bivalent oral polio vaccine (bOPV) – protects against poliovirus types 1, and 3
- Monovalent oral polio vaccines (mOPV1, mOPV2 and mOPV3) – protect against each individual type of poliovirus, respectively
WHO https://www.who.int/en/news-room/fact-sheets/detail/poliomyelitis
WHO Polio Vaccine Information https://www.who.int/ith/vaccines/polio/en/
WHO https://www.who.int/csr/don/27-february-2019-polio-indonesia/en/